Summary
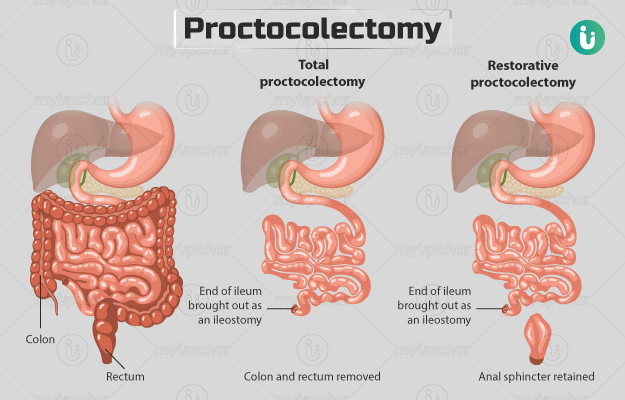
Proctocolectomy is a surgery in which the colon and rectum are removed. The colon, rectum and anus are parts of the large intestine that serves in the elimination of faeces. In conditions such as cancer and inflammatory bowel disease, these organs become diseased and may need to be removed. Proctocolectomy can be total (removal of colon, rectum, and anus) or restorative (the colon and rectum are removed, and anus is preserved). After removal of the organs, an opening may be made on the abdomen (ileostomy) through which the waste is collected.